Revenue cycle management (RCM) is the process healthcare organizations use to handle the financial side of billing and collecting revenue for medical services. RCM starts when a patient books an appointment and ends when the balance is fully resolved through insurance payments, adjustments, write-offs, or patient payments.
RCM strengthens revenue by reducing claim denials, lowering days in accounts receivable, and increasing collections. This allows healthcare providers to get correct and timely payments and improve financial performance. A strong RCM process also helps organizations meet regulatory rules and improve patient satisfaction.
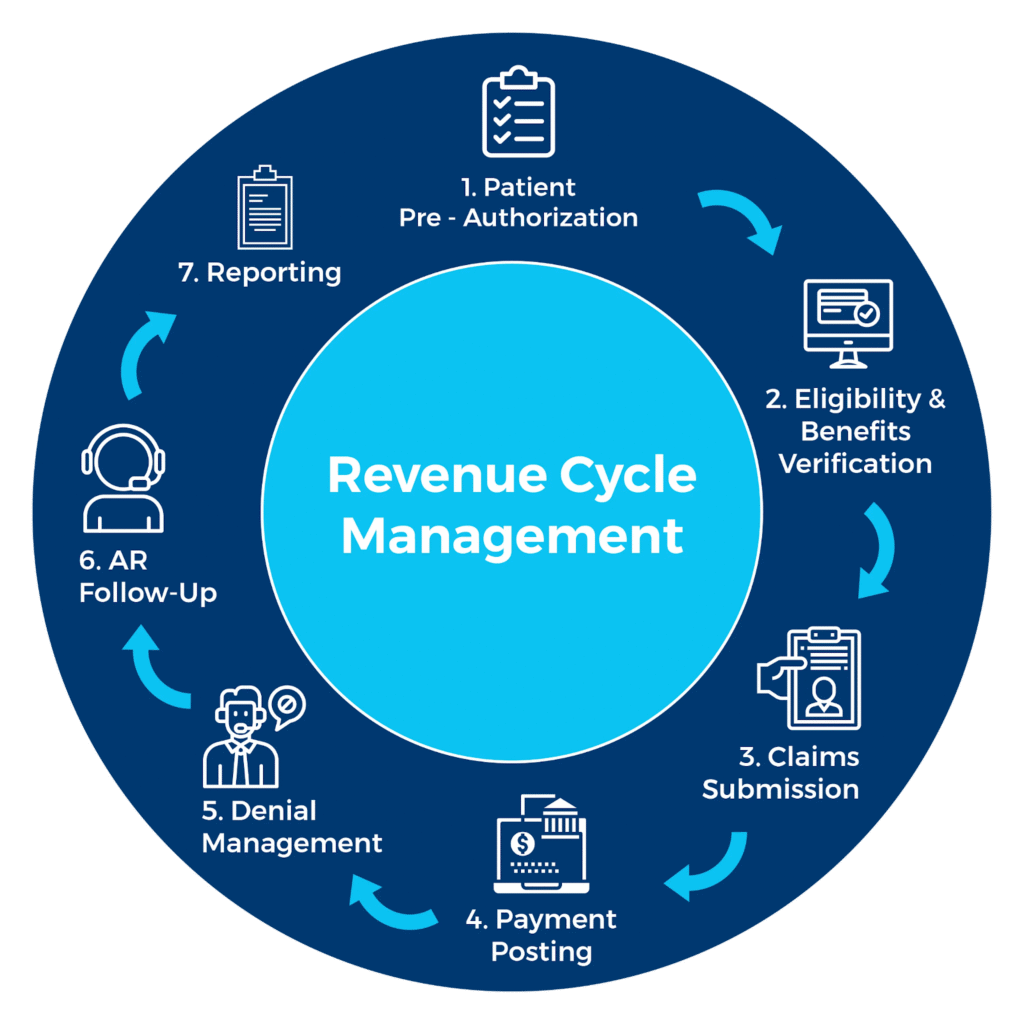
Steps for an Effective Revenue Cycle Include:
Appointment scheduling: Identifying service needs and collecting patient name, contact details, and insurance information.
Registration: Completing intake, verifying insurance, collecting payments at the front desk, and capturing demographic data.
Charge capture for services: Assigning medical procedure and diagnosis codes.
Billing: Creating clean claims for insurers and sending bills to patients.
Denial management: Reviewing denial reason codes to understand why claims were denied and correcting errors to prevent future denials.
Accounts receivable (A/R) follow-up: Identifying and following up on unpaid claims.
Each step has many tasks and possible variations. For example, some services require prior authorization, mostly surgical or high-cost services where payers require approval before treatment.
What Is the Overall Goal of RCM?
RCM aims to increase and ensure accurate revenue by finding problem areas and improving or removing them. Effective revenue cycle management also helps providers address compliance issues such as fraud, waste, and abuse. For example, a practice might discover that unnecessary tests are being ordered, and can correct this to follow compliance rules.
Why Healthcare RCM Is Important
RCM is essential whether it is done in-house or by a revenue cycle management services provider. Without proper RCM, healthcare organizations may lose reimbursement, putting the entire facility at risk. Because of this, RCM affects how the healthcare industry functions every day.
Benefits of Healthcare RCM
RCM connects the financial side of healthcare with clinical care. It links demographic data (patient name, insurance provider, etc.) to the treatment a patient receives.
A strong RCM system streamlines billing and collections by accurately preregistering and scheduling patients, collecting balances, processing payments, and managing denied claims.
Healthcare teams (providers, managers, billers, coders, and preauthorization specialists) communicate using EHRs and accounting systems. RCM software helps them use EHRs more easily. This reduces admin costs and shortens the time between providing a service and receiving payment.
RCM systems also help staff enter required claim information correctly, reducing the need to revise or resubmit claims. Fewer denied claims means less cost and time wasted.
RCM improves patient experience because insurance eligibility verification tells patients about balances before their visit. Accurate billing and coding lead to fewer denials and less confusion for patients and providers.
RCM systems allow patients to pay bills online and help providers manage billing records.
RCM depends on accurate documentation to show medical necessity. Better documentation supports better care and improves patient safety. Most clinicians review charts to ensure clear documentation.
RCM systems also simplify reporting and data analysis, helping organizations monitor how well the revenue cycle performs.
Challenges Associated With Healthcare RCM
Revenue cycle management is complex because of coding, billing, compliance, credentialing, data analytics, and working with paper charts alongside EHRs.
RCM Challenge 1: Coding Precisely and Billing Accurately
Accurate coding and billing are separate tasks, but both are essential for proper payment. Coders extract billable data and assign ICD-10-CM, CPT®, and HCPCS codes, while billers submit claims using those codes.
Coding and billing mistakes lead to denied claims and lost revenue because staff must fix and resubmit claims, increasing office costs. Organizations may have one person do both tasks, or separate roles, or outsource medical billing and coding to a trusted company.
Coders must ensure documentation supports assigned codes and verify procedure codes, diagnosis codes, insurance, and provider details. Both billers and coders need updated knowledge of rules, guidelines, payer requirements, and frequent changes. Organizations should test their skills, train them regularly, and may require drug screenings.
RCM Challenge 2: Meeting Compliance Standards
Healthcare compliance prevents fraud, waste, and abuse. Under HIPAA, organizations must protect patient data and avoid unauthorized disclosure. Failure to follow compliance rules can lead to fines up to $1 million.
RCM must follow strict coding standards, perform audits, follow claim-filing rules, and maintain HIPAA-compliant workstations.
RCM Challenge 3: Credentialing Providers
Provider credentialing connects providers with payers for approval. Without credentialing, payments are delayed or denied. Practices need a credentialing specialist to manage required documentation and verification.
RCM Challenge 4: Applying Data Analytics
Data analytics involves reviewing reports on denials, charges, reimbursements, and more to find trends, errors, and missed billing opportunities. Fixing these issues improves revenue, accuracy, and efficiency.
RCM Challenge 5: Incorporating Paper Charts
Paper charts do not integrate with EHRs, limiting access to patient information and causing incomplete documentation for coders and auditors. This affects claim accuracy and patient care quality.
How to Improve Revenue Cycle Processes in a Clinic or Physician Practice
Clinics can improve RCM by reviewing each step to find strengths and weaknesses. Data analytics provides facts to support decisions.
Every step is connected, so errors in one area cause issues in others. Hiring a qualified RCM manager helps unite front-end (registration, eligibility, precertification) and back-end processes (claims, denials, billing, collections).
Front-end steps that support back-end success include:
- Correct patient information at scheduling and registration to avoid claim denials.
- Verifying eligibility to confirm coverage before the appointment.
- Managing prior authorization carefully to avoid lost revenue.
- Working with providers on peer-to-peer reviews when payers require clarification.
- Ensuring communication between clinical documentation staff and billing staff.
Additional steps to improve RCM include:
- Staying current with coding and guidelines.
- Using edits to catch coding and reporting errors.
- Having a compliance liaison to audit charges.
- Working denials on time and in groups for efficiency.
- Using technology to streamline processes.
How to Know Whether Your RCM Is Performing Well
Data helps evaluate RCM whether done in-house or outsourced. Important healthcare RCM financial and performance benchmarks include:
- Point-of-service (POS) collections: Tracks copayment revenue.
- Days in accounts receivable: Measures how long it takes to collect payments.
- Days in total discharged not billed: Shows delays in billing services already provided.
- Clean claim rate: Measures clean billing with fewer errors and denials.
- Bad debt: Shows uncollectible debt and how effective collections are.
Read More Gorod








